Jeff Merchant of Terry had been hunting some 47 years.
So on Nov. 4, he felt confident as he climbed to put new straps on a lock-on tree stand.
It was the proverbial pride before a fall.
“The top of the stand broke and pulled my feet off the section I was standing on,” he said. “I fell 19 feet.”
He landed standing up, dislocating both ankles and crushing his heels. Then he fell backwards atop his bow.
To find help, he arm-crawled toward his father’s house, about a half-mile away. “I had to have my feet in the air, and they were just flopping they were so broken,” he said. “It was 400 yards before I got cell service.”
He sent his father the shortest text he could think of: “I am hurt.” And soon he heard “the beautiful sound” of a four-wheeler headed his way. A fire department pick-up truck ferried him out of the woods, and an ambulance met him at his father’s house.
What followed was 10 surgeries (three on the right foot, seven on the left), multiple procedures to fight infections and enough pain to convince Merchant to cry uncle.
On Feb. 21, he had his left leg amputated at mid-shin.
“It’s a hell of a thing to say: ‘Doc, cut my leg off,’” he said. “Afterward, I said it was the smartest thing I did. I wish I’d done it four surgeries before, but you want to save the foot.”
Ultimately, Merchant had “an unrecoverable injury” due to damage to the soft tissue and muscles in his left foot, said Dr. Peter Arnold, a board certified plastic surgeon at the University of Mississippi Medical Center who specializes in complex traumatic and surgical wound reconstruction.
Arnold said it was no easy task to tell Merchant the bad news. “It’s always a challenging conversation. Everyone on my team sits down with them, and we go through it and have a long talk. We say our goal is to get you the best function that we can. There’s a lot you can do with a properly fitted lower extremity prosthesis.”
And what occurs in the operating room impacts fit and function.
“One of my professors used to say a below-the-knee amputation is one of the most difficult and most important operations we do,” Arnold said. “What you are doing in the operating room, patients live with for the rest of their lives.”
Fortunately, less are living with phantom pain, a condition where people with amputations perceive pain coming from a limb that’s not there. Credit goes to a relatively new procedure called Targeted Muscle Reinnervation (TMR).
Arnold said TMR involves a different approach to handling nerves in the residual limb. Traditionally, he would pull out each nerve, tie it off, transect it and let it retract into the body. As a result, painful scar tissue sometimes developed around the end of the disconnected nerves.
Now, he connects the nerves to others that are still attached to muscles. “The simplest way I can explain it is we give those nerves a job,” Arnold said. “And it seems to dramatically decrease phantom limb sensation and phantom limb pain.”
Today, Merchant’s lack of phantom pain has helped him stay focused on saving his lifestyle, a mission that brought him to Methodist Rehabilitation Center’s Flowood campus.
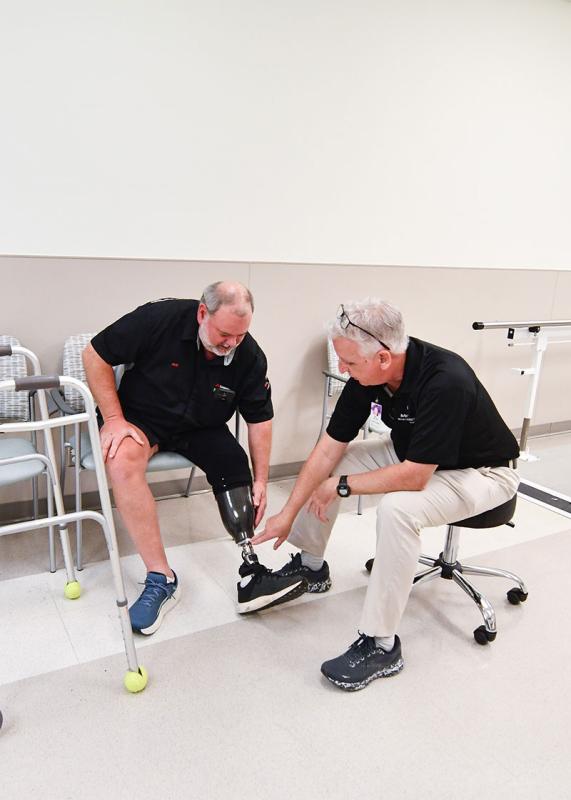
It’s home to Methodist Orthotics & Prosthetics, where he was custom-fit with a prosthetic leg. Across the hall is Methodist Outpatient Therapy, where he’s learning how to walk with the new limb.
Like Arnold and his peers at UMMC, Methodist staff stay abreast of innovations. Methodist O&P has launched many a new prosthesis in Mississippi, while the outpatient therapy division is usually first in line for new equipment and approaches to care.
But Merchant says convenience actually brought him to Methodist’s Flowood campus. He likes being seen in side-by-side clinics, where his care team can collaborate on problems common to new prosthetic users.
Just a few weeks into the process, Merchant had already made significant progress. He’s back at work as a freight operations supervisor for XPO Freight in Richland and recently went fishing from a friend’s boat.
Methodist certified prosthetist/orthotist Bret Lee said Merchant was obviously motivated. “I knew he’d do well the first day I met him because attitude is everything if you have good basic ability.”
Lee was mindful of Merchant’s high activity level as he chose components for his prosthesis. Its flex foot has the technology to store energy and return it to the user.
The leg also features a suction system activated by a tiny pump inside the foot. Every time Merchant steps on the pump, it creates a vacuum inside his socket. This keeps the leg attached to his residual limb. “It makes it feel more like a part of him,” Lee said.
As a below-the-knee amputee, Merchant hasn’t had the struggle of adjusting to a computerized knee. Still, he’s challenged by a right foot that’s full of hardware and often painful. “Most people have a good foot and a prosthesis,” he said. “I have half of a foot and a prosthesis.”
Lee is building Merchant a custom brace to bolster his right ankle and foot. In the meantime, Merchant is working with Methodist physical therapist Cameron Huff to fine-tune his walking ability.
“I told him he wasn’t going to believe how much easier it would be on a prosthesis than hopping on one leg,” Huff said. “And what I predicted was right. He took to it just like that.”
As Merchant got acclimated, Lee and Huff have made sure he understands the importance of taking care of his skin—particularly the point where the prosthesis meets the end of his residual limb.
“In some below-the-knee amputees, the weight bearing surface is the patellar tendon,” Huff explained. “And God did not mean that to be weight-bearing.”
To help avoid dangerous skin irritations, new prosthetic users are taught to gradually build up their tolerance to wearing the limb.
For the first week, Merchant wore his leg just two hours twice a day, with a two-hour break in between. He’ll continue to add an hour of wear time each week until he reaches the desired number of hours that would be a “normal” day for him.
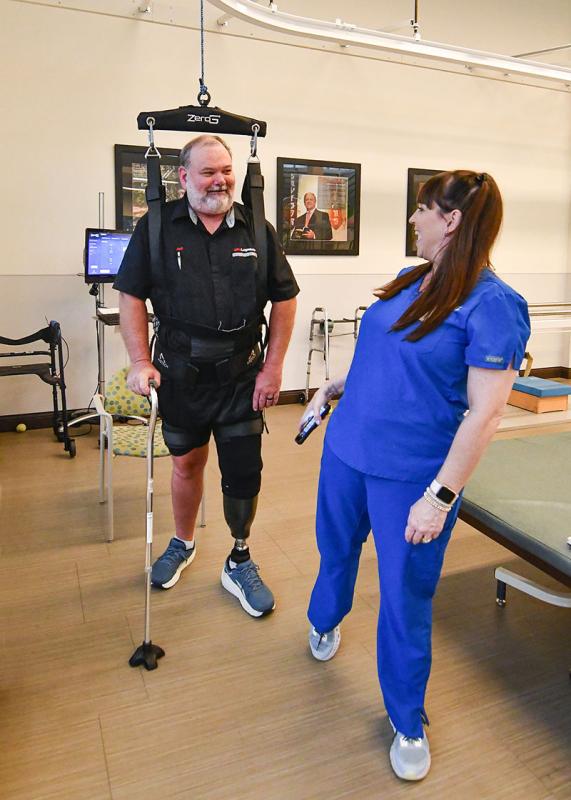
While wearing his prosthesis in therapy, Merchant has been practicing everything from stepping over hurdles and climbing steps to walking with the aid of Methodist’s ZeroG Gait and Balance System. The therapy aid features a supportive harness attached to an overhead track system, and MRC has two of only three such systems in Mississippi. It allows patients to practice walking, balance tasks, sit-to-stand maneuvers and climbing stairs without fear of falling.
“And it’s easier to try things when you know you can’t fall,” Huff said.
While Merchant walks, Huff focuses on where his feet should be during each phase of the gait cycle. “We want his new leg to function like his old leg,” she said. “But some of it is not 100 percent perfectly achievable.”
For instance, one goal is for Merchant to put the same amount of weight on each foot as he walks. But Huff said that’s difficult for him since he has no sensory input in either foot. “I can’t feel the bottom of my right foot, and I sure can’t feel the left,” he said.
Yet Huff said she has “no doubt” he’ll eventually walk unassisted. He’s already moved up from wheelchair to walker to cane.
The Holy Grail for Merchant is to be able to get back to hunting. “I take vacations to go to deer camp. It’s my stress relief,” he said.
Once he is back in the woods, Merchant has vowed to keep his feet firmly on the ground. “Climbing trees is over for me,” said the 60-year-old. “I’m too old for this to happen again.”
Arnold believes it’s a decision more Mississippians would be wise to make. “We see a lot of these kinds of injuries where people fall out of deer stands every year. They can be devastating,” he said.
Ten Tips for Tree Stand Safety
- Always wear a fall-restraint device. Wear it from the time you leave the ground until you return to the ground.
- Read and follow manufacturer’s instructions and warnings.
- Practice with your tree stand at a low level, under 5 feet, until you are sure you know how to use the stand.
- Check your stand before and after each use. Correct problems before using stand again.
- Take your time when climbing and watch every step you make.
- Never climb with anything in your hands. Use a pull rope to bring up equipment after you’re secure in your stand.
- Watch the weather. Some tree stands will slip on wet trees. Most stands are made of metal and are not safe during lightning storms.
- Do not sleep in tree stands or drink alcohol or take drugs during tree stand use.
- Tell someone exactly where you will be hunting and what time you plan to return. Agree that they will search for you if you do not return within an hour of that time.
- Take a whistle, flashlight, cell phone or two-way radio so you can signal rescuers with your location.
Source: “The User’s Guide to The Tree Stand (Its History and Safe Use)” by L.J. Smith